This is for informational purposes only. For medical advice or diagnosis, consult a professional.
When I first started this blog seven or eight years ago, writing about aneurysms was the last thing on my mind. But that was before I married Deena and well before she was diagnosed with a brain aneurysm of her own. I journaled about her adventure and successful surgery last summer HERE and about the occasionally bumpy road to recovery HERE. Little did I know that these two threads alone would have 1,500 views in just over six months time, making them among my most popular. As the first thread grew longer, I had to start a second and now I need to begin a third. What I hope to do in his post is to continue to share news and information on intracranial aneurysms in a way that most people can easily understand. I believe that “knowledge is power” and I hope to help you experience as someone who is possibly facing this or caring for someone with this diagnosis. I am a retired military medic who taught basic and advanced classes to other medics but I am most definitely not a physician. My second career as a college teacher cemented my desire to learn and share what I learn with others, and this is what motivates me. Some of what I learn is not readily available and I enjoy coaxing the professional literature for interesting and useful information. So, please do not act on whatever you read here. Follow the instructions of your family physician, your neurologist or your neuro-surgeon as you walk this path.
MONDAY, MARCH 3, 2025: Intracranial aneurysms and your mental health
First, a little background
Getting the news that you have an aneurysm in your head can be very scary. Personally, I have not idea how scary because I never had to deal with it myself. I can only emphasize based on Deena’s experience. Most of us know someone who has had a stroke. A stroke is the term used to describe a more or less and often catastrophic and irreversible loss of function, whether speech, vision, movement, sensation, awareness, cognitive abilities and so on. There are two common causes of stokes. The more common is a blockage in a blood vessel in the brain, The word “thrombosis” is usually used. More than three out of four strokes are the result of this blockage.
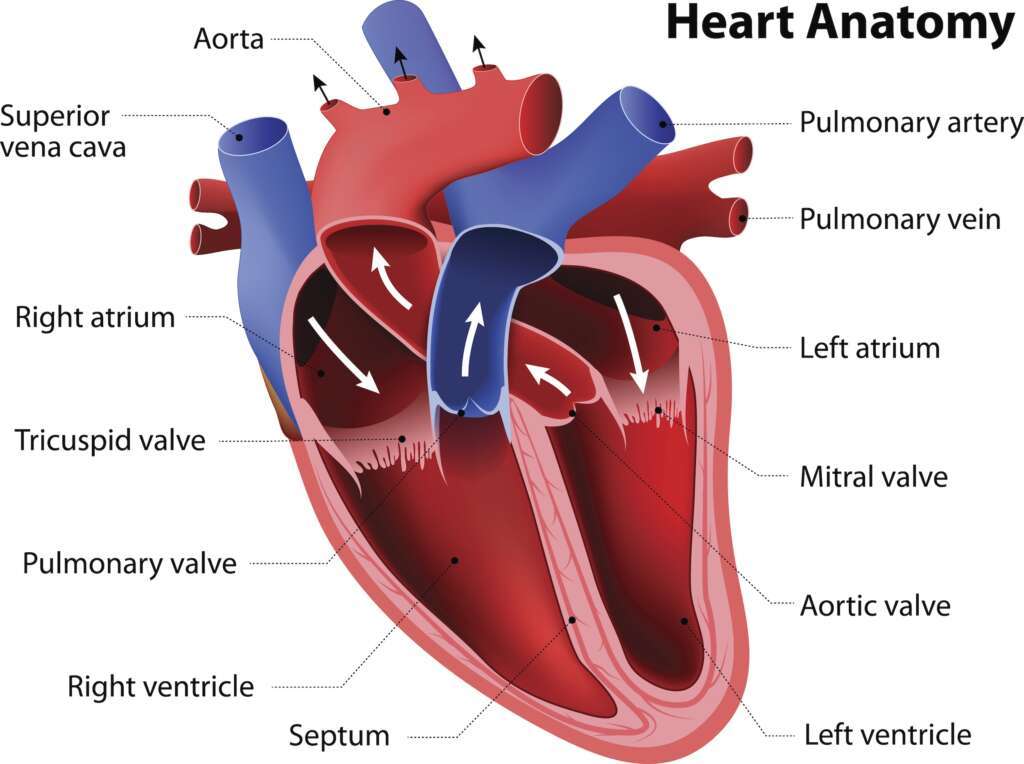
So, what causes this blockage? The first thing that comes to mind is a blood clot. Whenever blood does not circulate properly, there is a potential for a blood clot to form. You may know someone who has a sensation of fluttering or pounding in their chest around their breastbone. Often the term “palpitation” is used. When the doctor takes an EKG on this person, they may say that he or she has atrial fibrillation or some other atrial rate disturbance. The atrium (see diagram) will not beat as normal and this presents the opportunity for a small clot to form, which may eventually wind up in the brain. At first, the clot may move freely in the artery as it leaves the heart, but as the artery gets smaller and smaller, eventually it gets lodged in the blood vessel and blood cannot pass by. Once the clot lodges, the brain tissue downstream is deprived of blood and nutrients and dies. This process is like leaves in autumn blocking a storm drain on your street. At first, some water may pass but eventually, there is a flood. So, interventional cardiologists have a number of treatment options that I won’t mention here, but one concern is clot formation, so they often prescribe a blood thinner which makes it more difficult for blood to clot. Blood thinners can be a nusiance to some patients but they are also life savers.
A second cause of blockage is when a tiny piece of plaque in an artery breaks off. As you age, you may acquire a buildup of cholesterol and other fatty substances, calcium and so on in your arteries. This is sort of like calcium buildup in your showerhead. Eventually the stream of water slows down. If the buildup occurs in the three cardiac arteries of your heart, you are at risk of a heart attack. Again, there are procedures to address this which I won’t go into.
If this piece of plaque lodges in an artery in your brain, it has the same effect as if it was a blood clot. It stops the flow of blood.
The cause of a stroke is when a blood vessel in the brain ruptures and this is typically called a cerebral hemmorhage. Some of the more common reasons for a cerebral hemmorhage are trauma (falls and accidents), a blood pressure high enought to rupture an artery in the brain, or an aneurysm where you have a built in weakness (bulging) in an artery which can tear over time.
Any amount of waiting–even a week before a spot in the surgical schedule opens up–can be and usually is stressful for a patient. This post, however, is written for the intracranial aneurysm patient who must wait indefinitely for even a decision to operate. So, this different than a breast cancer survivor “watching and waiting” for a possible reemergence of her cancer. Between her own breast self-examinations (BSE), visits to her physician, mammeograms, scheduled scans and what not, there is a good chance of detecting an emerging mass before it becomes life threatening. An aneurysm, however, can become lethal over night.
Now to the point
Much of the research and literature on aneurysms comes from or through the American Heart Association and the American Stroke Association. Last summer, they published an article (you can find here) on people who have brain aneurysms and while these patients are being monitored, they are not actively being treated with any form of invasive intervention. In most cases, it is because of the small size of the aneurysm. The current consensus is to not consider surgery as a first resort if the aneurysm is 5 mm or less in size (all things being equal), though there are caveats. Some surgeons do choose surgery for smaller sized aneurysms. Other considerations that neuro-surgeons ponder have to do with the risk of rupture of the aneurysm and the location of the aneurysm within the brain. Aneurysms on the posterior (i.e., rear) communicating artery, those aneurysms with irregular shapes and a patient with a previous history of a rupture or who has multiple aneurysms at the time of diagnosis may qualify for early intervention rather than surveillance over time. During your meeting, your neuro-surgeon, he or she may complete what is called a PHASES score on you. PHASES stands for “Population,” “Hypertension,” “Age,” “Size,” “Earlier . . .” and “Site.”
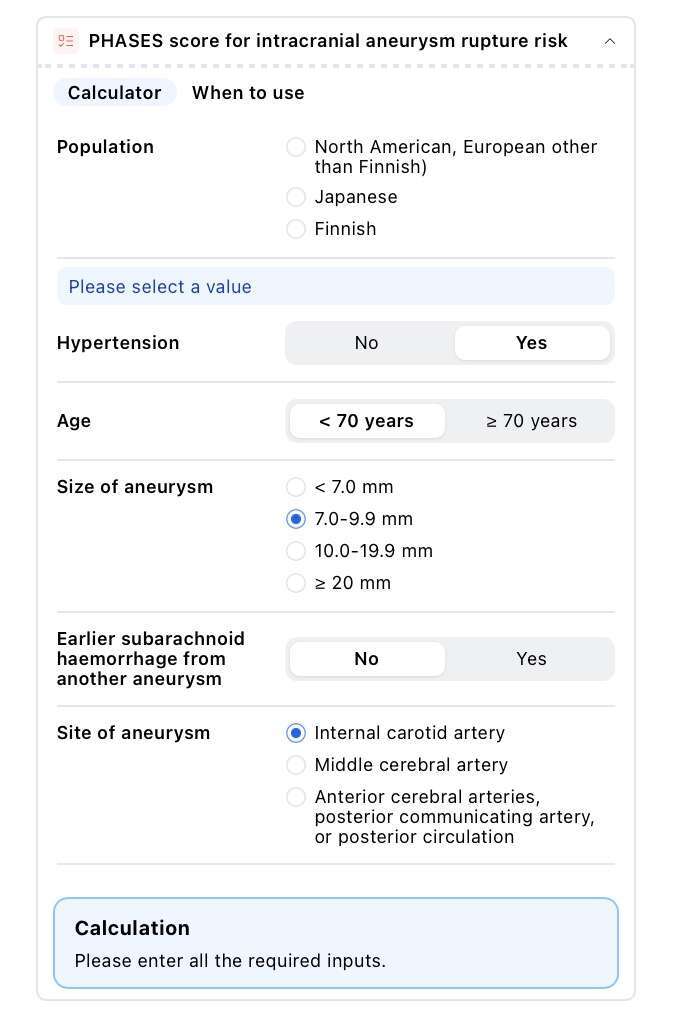
Once each of the six questions on the template are answered, the program creates a reasonable risk of rupture over the next five years. It is for you and your surgeon to weigh together the risks of waiting vis-à-vis moving ahead with treatment. If it were me, more often than not I would follow the advice of my surgeon, especially if he or she is experienced in this area and comes with high recommendations.
One last reason not to do surgery is when there is a more than an acceptable risk of injury or loss of life were a surgeon to attempt to repair the aneurysm. So, these people wait. They go to sleep each night not knowing if they will wake up in the morning. Or, they have unusual senations or headaches that suggest to them something bad is happening–maybe their aneurysm is about to burst?! They don’t know what they can safely do. Can they exercise? Can blowing their nose forcefully or will vomiting or coughing affect their aneurysm? Can they fly? Overtime, a creeping sense of fear, anxiety and occasionally dread may set in and can actually disturb their lifestyle, even among the most emotionally stable of them. By “this”disturb” I mean create problems at work or school, their plans, even their relationships (including marriage.) Waiting is definitely not easy.
So, as expected, this study warns of an increased mental health vulnerabily, even if and especially if, there was no suggestion of mental health problems before the aneurym was detected. And the age group most affected are people forty years of age and younger. That is perfectly understandable. I’ve read of young women thirty-something with an aneurysm and they wonder what will happen to their ability to care for their children if their aneurysm ruptures? In fact, I knew a single mom in my church years ago with twin eight-year old boys. When I saw her a few weeks after her hemmorhage, she was conscious, but bed ridden and could not speak. Yet, her eyes spoke for her. I could see the anguish and loss clearly. How could she be a mother anymore? How could she even allow her children to see her this way without frightening them?
The ten-year study conducted in South Korea concluded:
- People diagnosed with unruptured cerebral aneurysms (weakened areas in brain blood vessels) who are being monitored without treatment have a higher risk of developing mental illness compared to those who have not been diagnosed with a cerebral aneurysm. The largest impact was among adults younger than age 40.
- The study conducted in South Korea found that the psychological burden caused by the diagnosis of an unruptured aneurysm may contribute to the development of mental health conditions, such as anxiety, stress, depression, eating disorders, bipolar disorder, insomnia and alcohol or drug misuse over a 10-year period.
- The researchers suggest providing support to help patients cope with the stress of the diagnosis may be an important part of comprehensive care.
- In cases where a [pre-existing] mental health condition was diagnosed by a psychiatrist, the difference was even greater, showing a three-fold increased risk.
The study noted that even when the aneurysm was too small to justify an operation, the fact that it was there at all was enough to heighten fears of a rupture, even when the patient was repeatedly assured that the risk of a rupture was statistically very low. It does not take a patient on a computer very long to search and discover that up half of ruptured brain aneurysms are fatal, often with little or no warning (and I have discussed signs and symptoms of this event elsewhere in my aneurysm threads.) And a good deal of those who survive have significant neural deficits for the rest of their lives.
A report in Medical News Today from May 2023 goes even further. They report that signs and symptoms of schizophrenic behavior (including paranoia) and difficulty maintaining an emotional balance can occur as well. It is possible that a slow growing aneurysm can put pressure on surrounding blood vessels and tissues which can trigger psychological issues, but then that would be a reason to attempt surgical correction if surgery were a viable option in the first place.
If might be worthwhile getting the opinion of others, particularly those who have gone through the surgery and possibly those who did not but who wished that they had.
WEDNESDAY, MARCH 5, 2025: Why some intracranial aneuryms are caused by family genes
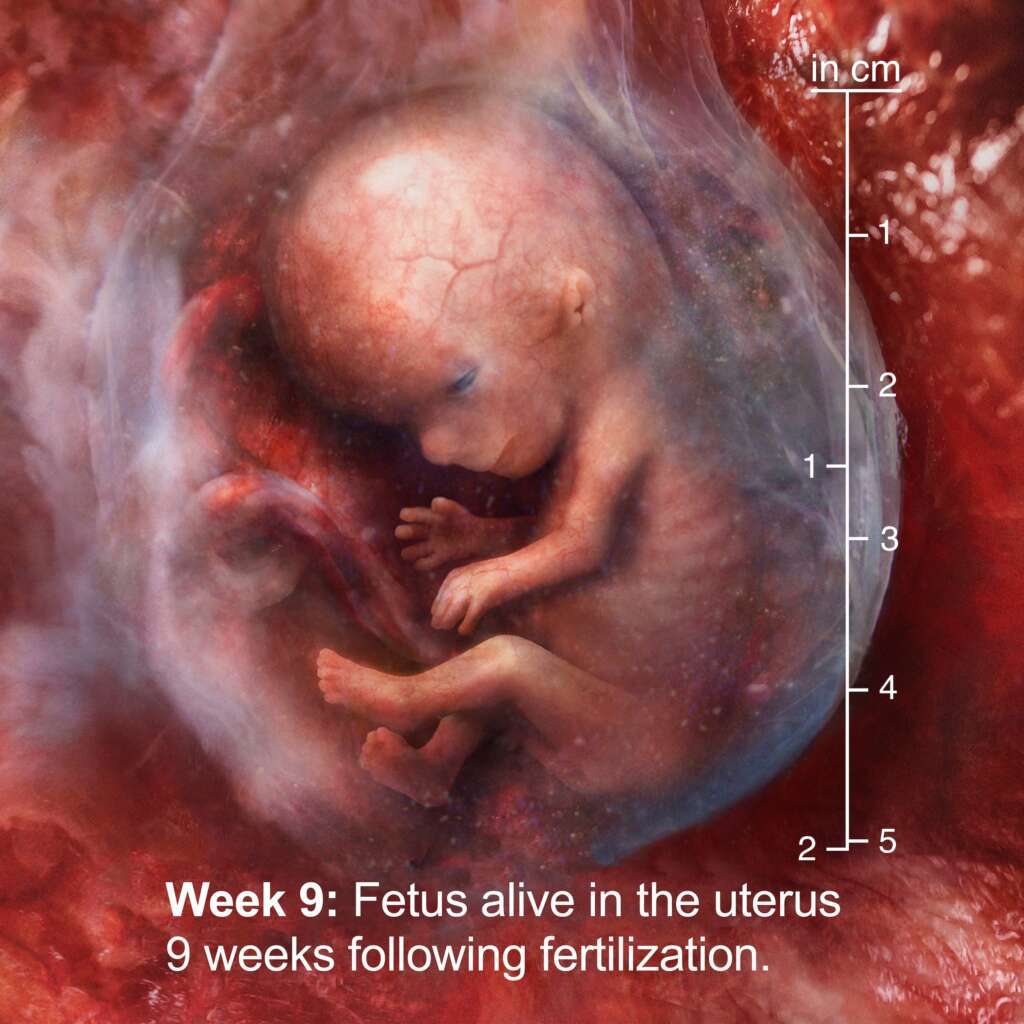
You can live a perfect life. You can keep your blood pressure under control. You can avoid smoking and the other risk factors that can lead to an intracranial aneurysm and still get one. This is because some aneurysms run in families. To understand this, let’s look at how the circulatory system in the brain develops.
The first evidence of circulatory development in the brain of the fetus begins around the seventh week. These early nondifferentiated (i.e., generic or not specifically characterized) blood vessels are actually a form of capillaries that are barely competent (developed) in terms of structure. By the time the entire arterial network develops, the existing blood vessels begin to mature starting with the posterior part of what will become the Circle of Willis, which shunts blood similiarly to the expressway loop around a major city. When the fetus is ten weeks old, the emerging fetal cerebral circulatory system of the brain defines different areas of the network by designating some blood vessels to be arteries and others to be veins. By the sixteenth week, the arteries start showing changes in the diameters of the blood vessels, with those that are “upstream” becoming larger in diameter than those that are downstream. By now, the fledging network is providing the developing brain tissues with oxygen and nutrients. If the pregnant mother consumes alcohol, this is where fetal alcohol syndrome begins. When arterial development does not progress normally, development problems may occur. These include everything from cognitive delays and abnormal motor function to a decreased size of the baby’s head.
The correct construction of the cerebral vascular system in a fetus depends on the genetic blueprint coded in the baby’s DNA. As a overly-simplified, less than apt example, imagine being shown around a brand-new house where light switches are installed on the ceiling, well out of reach, or electrical receptacles are mounted backwards in the wall so that they are useless. Doors may not have doorknobs or if they do, they may be on the edge of the door where the hinges are. Maybe the kitchen sink was mounted in the floor of the bedroom and the shower located on the front steps?
Every part of you from the color of your eyes to how well your body produces insulin to how many fingers you have on your hand depends on one or more genes. And it depends on them following the master genetic bluebrint correctly. Sometimes, there are replication errors or “glitches” in a gene and something does not turn our right. Maybe the blueprint for the new house calls for glue or beeswax to hold the frame together instead of nails. In that case, the house will start to come apart and it is the same with your body.
LOXL2: An example of how a faulty gene can lead to aneurysms later in life
There is a gene called LOXL2 on the eighth chromosome. Along with the ~699 others genes on this chromosome, and according to Pathway MD, the
“genes on the 8th chromosome are associated with a variety of functions including development of the nervous system, hormone production, blood cell development, and are implicated in conditions like certain cancers, heart defects, and developmental disorders.”
LOXL2 produces a protein that allows for an amino acid call lysine to be captured from a person’s diet. Foods such as red meats, fish, pork and poultry and cheese (particularly Parmesan cheese) are rich in lysine. Because our bodies do not actually manufacture lysine, it is important that we eat these foods and that our body captures the lysine, else we will not function normally. For the sake of simplicity, we need not be concerned here about proteins and amino acids, what they do, how they differ, etc.

When there is a deficiency in the ability of the gene LOXL2 to extract lysine from what you eat, this lack of lysine can lead to weakened arterial vessel walls, increasing the risk of aneurysm formation over time. If the gene was corrupted in the sperm or egg that produced you, your LOXL2 may be corrupted as well. This means you may not be capturing enough lysine for your artery wall to be able to resist bulging out to form aneurysms in sundry places in your brain when your blood pressure rises. This mutation of the gene LOXL2 on your eighth chromosome is called the LOXL2 c.C133T mutation.1 Seven other chromosomes in your body have genes that if corrupted, can form intracranial aneurysms at some point in your life. It you get these damaged genes from your parents (as opposed to being exposed to some mutagenic toxic chemical), you may quite possibly pass down this tendency to develop aneurysms to your children. And we’re only looking at intracranial (cerebral) aneurysms. Some of these corrupted genes are part of larger genetic disorders such as Marfan syndrome or Polycystic Kidney Disease.
Genetic testing can reveal if you have the genes for intracranial aneurysms, though frequently it can more cost efficiently be discovered when a parent and a sibling or offspring of that parent has an aneurysm. In the case of my wife Deena who inspired me to research this, her mother and her brother had an aneurysm as did she. Her neuro-surgeon advised her children to get checked as well as her other siblings. It’s possible that her grandchildren may someday be at risk.
I hope I haven’t been too technical here because genetics is not an easy field. I just wanted to provide just one example of how the propensity to develop aneurysms can pass down through the genes.
FOOTNOTES
1A few of the other consequences from this singular corruption. From Pathway MD (passim):
“The LOXL2 c.C133T variant refers to a specific genetic change in the LOXL2 gene, which may have implications in various biological processes, including fibrosis and cancer progression. Understanding this variant can aid in research and potential therapeutic developments.
Significance of LOXL2 c.C133T – The LOXL2 c.C133T variant has been identified as a pathogenic mutation responsible for a fraction of familial intracranial aneurysms.
Tumor progression: LOXL2 is involved in various cancers, including clear cell renal cell carcinoma (ccRCC) and non-small cell lung cancer (NSCLC), where it plays a role in tumor progression and metastasis.
Functional role of LOXL2 – LOXL2 functions as an amine oxidase, promoting cross-linking in collagen and elastin, which is crucial for extracellular matrix remodeling.
Prognostic factor: High LOXL2 expression is associated with poor prognosis in various cancers, including gastric and colon cancer.”
FRIDAY, MARCH 7, 2025: Dogs and cats can get intracranial aneurysms as well
Intracranial aneurysms are occasionally found in dogs or cats. Not surprisingly, the signs of a ruptured cerebral are the same as one finds in people. These include (in dogs):

- Bleeding from ears or nostrils
- Blue skin
- Loss of consciousness
- Rapid breathing
- Seizures
- Sudden death
- Unusual posture
Cats would likely have similar signs as dogs. Of course, there is no way of knowing if they have “thunderclap” headaches, visual disturbances or anything like that since they cannot report how they are feeling. As a result, the only indication that a pet might have an aneurysm is when it ruptures and the pet dies (often in a matter of minutes.). The know causes of intracranial aneurysms in dogs and cats are those that are common among people, including hypertension, injury, infection and arteriosclerosis.and so on. Surgical intervention to iresolve anuerysms in dogs and cats is generally not attempted because their blood vessels are so thin.
TUESDAY, APRIL 15, 2025
Deena has had nosebleeds (episodes of epistaxis) three or four times during the past few weeks. They usually appear when she’s sleeping, but yesterday she had one while reading while in the living room. It’s always from the right nare (i.e., nostril.) We were able to rule out the typical things like sinusitis, trauma to the nose, high blood pressure and anticoagulant therapy (though she must still take 82 mg of aspirin daily for the rest of her life.) We plan to get her to and ENT doctor in case there are polyps, etc. But I suppose it could be the aspirin, and we cannot discontinue that without a risk of a cerebral blood clot. Plus, it would be contrary to the doctor’s orders. I suppose that if the epistaxis problem continues, we can check with the neurologist surgeon. He might be able to swap out a prescription drug that suppresses clots but does not cause bloody noses? Or, she may have to put up with it, which is a small price for avoiding a stroke.
No more problems with optical issues such as scintillating scotoma.